On 19 July 2022, NCITA hosted the fourth lecture in the NCITA ‘On the Shoulders of Giants’ educational lecture series: ‘Striving for Evidence - With and Without a Randomised Controlled Trial’ with Professor Tom Treasure, Cardiothoracic Surgeon and Honorary Professor in the Clinical Operational Research Unit at University College London.
In this lecture, Professor Tom Treasure demonstrated the importance of understanding the evidence behind well-known interventions before we accept them as standard practice, using pulmonary metastasectomy in colorectal cancer, and aortic root replacement for Marfan syndrome as two powerful examples.
To watch a recording of the event please visit the NCITA YouTube channel.
The perpetuation of a flawed belief: Pulmonary metastasectomy in colorectal cancer
If bowel cancer spreads to the lungs, patients can have a pulmonary metastasectomy - surgery to remove the metastases in the lung - which is thought to improve survival but can affect quality of life. Whilst operating to remove lung metastases slipped into surgical practice about 40 years ago, there is a low level of evidence to support the belief that pulmonary metastasectomy improves survival.
Recognising the low level of evidence, The Society of Thoracic Surgeons formed a task force and in 2019 published an expert consensus on Pulmonary Metastasectomy. Whilst providing a number of recommendations for Pulmonary Metastasectomy, they noted that whilst there had been over 1,000 publications, no randomised controlled trials were performed. Most of the previous studies were usually from a single institution and included single or multiple pathologies where metastatic disease survival was assumed to be zero, and survival gain (5YS) is believed to be ~40%.
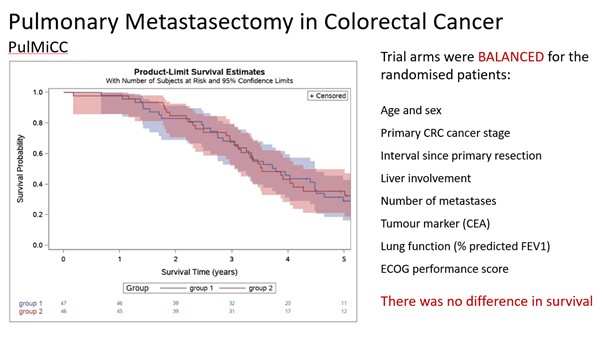
The Pulmonary Metastasectomy in Colorectal Cancer (PulMiCC) trial, of which Professor Treasure was Chief Investigator, was a randomized multicentre controlled trial which tested the effectiveness of Pulmonary Metastasectomy by comparing active monitoring with or without metastasectomy. The study contradicted a number of these beliefs from the expert consensus on Pulmonary Metastasectomy: 1) A randomised controlled trial was available, 2) Control survival was not zero, and 3) Survival gain was not ~40%.
Also relevant to the PulMiCC trial were the results of the carcinoembryonic antigen (CEA) Second-Look Trial, a randomised controlled trial that started in 1982 and remained unpublished for 20 years. A CEA test is often carried out after surgery for patients with bowel cancer. If CEA level is raised and metastases are detected in the liver or lungs, patients are assessed for surgery to remove the metastases. The lack of clarity in whether this resulted in better survival for patients led to the CEA Second-Look Trial. Under the Restoring Invisible and Abandoned Trials (RIAT) initiative, the trial data was recovered by Professor Treasure and colleagues. The data of the CEA Second-Look Trial were analysed and published in the BMJ, concluding that it was highly unlikely that any survival advantage would be demonstrated for CEA prompted second-look surgery.
These studies demonstrated the importance of randomised controlled trials to provide the evidence to challenge established procedures. Through the PulMiCC trial and CEA Second-Look Trial, the results found no indication of an important survival benefit from metastasectomy, and challenged the assumption that people with bowel cancer which has spread to the lungs should have a metastasectomy to improve their survival.
Challenging the norm: Marfan syndrome
Marfan syndrome is an inherited disorder that affects the body’s connective tissues, including the heart and blood vessels. The aorta tends to widen and enlarge over time, and can be life-threatening. Since 1968, operative resection and replacement of the aorta has saved many lives and extended survival, where the immediacy of a mechanistic benefit has been accepted as evidence enough; however, the operation requires life-long anticoagulation which has associated risks of bleeding and thromboembolism.
In 2000 Professor Treasure was the guest speaker at a meeting of the Marfan Association when Taliesin Golesworthy, a professional engineer with inherited Marfan syndrome, challenged the established operative procedure, arguing that the risks were too high. He suggested that modern computer assisted design and manufacture might improve on ‘our cut-and-saw methods’.
His challenge to the accepted norm led to the PEARS (Personalised External Aortic Root Support) procedure. A 3D printed ‘sleeve’ of the patient’s own aorta modelled by computer-aided design (CAD), PEARS is made of medical grade knitted mesh which supports and prevents further enlargement of the aorta. In 2004 Taliesin was the first to have his proposed operation, and his aorta has remained unchanged since.

“Tal looked me straight in the eye and said, ‘Why don’t you surgeons get up to date and use CAD modelling and RP?’. Well, I had to admit I was stumped - I didn’t know what those things meant - so I said, ‘Well look, let me take a few questions that I might be able to answer, and let’s find each other over coffee’. […] The CAD model he was talking about is Computer-Aided Design, and from that, RP, which is Rapid Prototyping, to make a replica of his aorta, and then on that fashion this mesh which is already tried and tested – it is soft, pliable and has a pore size of .6 of a millimetre so microscopic structures - fibroblasts - can grow into it.” Professor Tom Treasure
Professor Treasure and his colleagues repeatedly explored the possibility of a randomised controlled trial, but two key decision-making factors based on patient preference stood in the way – the timing of the surgery, and the acceptance or avoidance of lifelong anticoagulation. Consequently, the IDEAL framework, used for evaluations of surgical innovations, was utilised.
IDEAL follows a distinct development pathway - Idea, Development, Exploration, Assessment and Long-term study. From the Idea in 2000 (proposal of modern computer assisted design and manufacture by Taliesin Golesworthy), to Exploration in 2014 (the first ‘in-man’ operation), as of 2022 this surgical innovation is at Long-Term study, including big data analysis, meta-analysis and microsimulation of lifetime event risks for all methods. Whilst uptake has been slow, and the procedure still considered as experimental by many, there have now been almost 700 PEARS operations carried out by 31 teams in 12 countries.

The Scout Mindset
Professor Treasure challenged the belief that pulmonary metastasectomy improves survival, through the PulMiCC trial and CEA Second-Look Trial. Taliesin Golesworthy challenged the established operative resection and replacement, using his knowledge of CAD modelling to lead to a new surgical innovation for Marfan syndrome.
“If you see, hear, read, or are taught something “that doesn’t look right”, 1) Question it, 2) Check the evidence behind it, 3) If it’s inadequate, put it to the test.” Professor Tom Treasure
Professor Treasure encourages us all to adopt the Scout Mindset – the ability to recognize when you are wrong, to test your assumptions and change course accordingly. His key takeout from this lecture: If you see, hear, read, or are taught something “that doesn’t look right”, 1) Question it, 2) Check the evidence behind it, 3) If it’s inadequate, put it to the test.

About the speaker
Professor Tom Treasure was a consultant Cardiothoracic Surgeon at The Middlesex and University College Hospitals in the 1980s, St George’s in the 1990s, Guy’s Hospital in the noughties and since 2007 has been an Honorary Professor in the Clinical Operational Research Unit, UCL, his present affiliation. He has a London University Master of Surgery and Doctor of Medicine for experimental research theses. Throughout his clinical career he has run funded randomised controlled clinical studies, and randomised patients into multicentre trials led by others. Later he was Chief Investigator on his own trials. Prof. Treasure was elected to the Council of the Royal College of Surgeons and was President of the European Association of Cardio-Thoracic Surgery.
About the ‘On the Shoulders of Giants’ lecture series
‘On the Shoulders of Giants’ is a series of educational talks where experts bring their perspectives to encourage and challenge wider thinking within the cancer imaging research community. See below for other lectures in the series:
- April 2022: ‘Screening for Cancer: The Good, The Bad and The Ugly’ with Prof. Michael Baum. Link to blog & recording here.
- May 2022: ‘Is Pursuing ‘a Passion for Science’ a Position of Privilege?’ with Dr Heather Williams MBE. Link to blog & recording here.
- June 2022: ‘Academia & Industry: What are the Ingredients for Successful Collaborations?’ with Kieran Murphy and Prof. Evis Sala. Link to blog & recording here.
- September 2022: ‘Talking with patients about sad, bad and just plain difficult things’ with Prof. Dame Lesley Fallowfield, Wednesday 21 September 2022 14:00 – 15:00 BST. Link to further information and registration here.


